Step right up to explore the world of Plantar fasciitis treatment options! Get ready to dive into a treasure trove of information that will help you banish foot pain for good.
Learn about the causes, symptoms, and various treatment options available to tackle this common foot condition head-on.
Overview of Plantar Fasciitis
Plantar fasciitis is a common condition that causes pain in the heel and bottom of the foot. It occurs when the plantar fascia, a thick band of tissue that connects the heel bone to the toes, becomes inflamed or irritated. This can lead to stabbing pain with the first steps in the morning or after long periods of standing or sitting.
Causes and Risk Factors
- Overuse or repetitive strain on the plantar fascia from activities like running or standing for long periods.
- Wearing unsupportive shoes or high heels that do not provide proper arch support.
- Being overweight or obese, which puts extra pressure on the feet.
- Tight calf muscles or Achilles tendon, which can affect the alignment of the foot.
- Flat feet or high arches, which can lead to abnormal foot mechanics and strain on the plantar fascia.
Symptoms of Plantar Fasciitis
- Sharp or stabbing pain in the heel or arch of the foot, especially in the morning or after activity.
- Pain that improves with rest but worsens with weight-bearing activity.
- Tenderness or inflammation along the bottom of the foot.
- Difficulty walking or standing for long periods due to foot discomfort.
- Stiffness or tightness in the heel or calf muscles.
Non-Surgical Treatment Options
When it comes to managing plantar fasciitis, non-surgical treatment options play a crucial role in providing relief and improving symptoms without the need for invasive procedures.
Physical Therapy
Physical therapy is a common non-surgical approach for treating plantar fasciitis. It involves targeted exercises to strengthen the muscles in the foot and ankle, improve flexibility, and reduce pain. Additionally, physical therapists may use techniques such as ultrasound or massage to help alleviate symptoms.
Orthotic Devices
Orthotic devices, such as shoe inserts or custom orthotics, can provide support and cushioning to the foot, helping to distribute pressure more evenly and reduce strain on the plantar fascia. These devices can also help correct abnormal foot mechanics that may contribute to the development of plantar fasciitis.
Stretching Exercises
Stretching exercises are an essential component of non-surgical treatment for plantar fasciitis. Specific stretches targeting the calf muscles, Achilles tendon, and plantar fascia can help improve flexibility, reduce tightness, and alleviate pain. These exercises are often recommended as part of a comprehensive treatment plan.
Surgical Treatment Options
When non-surgical treatments fail to provide relief, surgical interventions may be considered to address plantar fasciitis. These procedures are typically reserved for severe cases or when conservative methods have been exhausted.
Plantar Fascia Release
Plantar fascia release is a common surgical procedure for plantar fasciitis. During this surgery, the tight plantar fascia tissue is partially cut to relieve tension and reduce pain. This procedure aims to improve flexibility and reduce inflammation in the affected area.
Tenex Procedure
The Tenex procedure is a minimally invasive surgical technique used to treat chronic plantar fasciitis. It involves using ultrasound guidance to remove damaged tissue from the plantar fascia tendon. This procedure is less invasive than traditional surgery and typically results in a quicker recovery time.
When Surgery Might Be Considered
Surgery for plantar fasciitis is typically considered as a last resort when non-surgical treatments have been ineffective. It may be recommended for patients with severe pain that limits daily activities or when conservative treatments have not provided relief after an extended period.
Success Rates, Risks, and Recovery
The success rates of surgical treatments for plantar fasciitis vary depending on the procedure performed and the individual’s specific case. While many patients experience significant pain relief and improved function after surgery, there are risks associated with any surgical procedure, including infection, nerve damage, or prolonged recovery time. Recovery from plantar fasciitis surgery can take several weeks to months, and physical therapy may be recommended to aid in rehabilitation and restore strength and flexibility in the foot.
Integrative Approaches
Acupuncture, chiropractic care, and shockwave therapy are just a few examples of complementary and alternative therapies that can be used in conjunction with traditional treatments for plantar fasciitis. These integrative approaches aim to provide a holistic approach to healing and pain relief, addressing not only the symptoms but also the underlying causes of the condition.
Acupuncture
Acupuncture involves the insertion of thin needles into specific points on the body to help relieve pain and promote healing. Many individuals with plantar fasciitis have reported reduced pain and improved mobility after receiving acupuncture treatments. By targeting energy pathways in the body, acupuncture can help to improve circulation, reduce inflammation, and stimulate the body’s natural healing processes.
Chiropractic Care
Chiropractic care focuses on the alignment of the spine and musculoskeletal system to alleviate pain and improve overall health. Chiropractors may use spinal adjustments, massage therapy, and exercises to help individuals with plantar fasciitis achieve pain relief and improved function. By addressing imbalances in the body, chiropractic care can help to reduce stress on the feet and ankles, leading to better outcomes for those suffering from plantar fasciitis.
Shockwave Therapy
Shockwave therapy involves the use of high-energy soundwaves to stimulate healing in damaged tissues. This non-invasive treatment can help to reduce pain and inflammation in the plantar fascia, promoting tissue regeneration and improved function. Many individuals have found relief from chronic plantar fasciitis symptoms after undergoing shockwave therapy sessions. By targeting the affected area with focused energy, shockwave therapy can accelerate the healing process and improve outcomes for patients.
Relationship Between Plantar Fasciitis and Foot Health
Plantar fasciitis can significantly impact overall foot health and mobility. The condition causes inflammation and pain in the plantar fascia, the tissue that runs along the bottom of the foot, leading to discomfort and difficulty in walking or standing for long periods.
Preventive Measures for Healthy Feet
- Avoid wearing unsupportive footwear, such as high heels or flip-flops, which can strain the plantar fascia and increase the risk of developing plantar fasciitis.
- Maintain a healthy weight to reduce pressure on the feet and lower the risk of developing foot conditions.
- Engage in stretching exercises for the feet and calves to improve flexibility and prevent tightness that can contribute to plantar fasciitis.
Importance of Proper Footwear and Care
- Choose shoes with adequate arch support and cushioning to provide proper alignment and reduce strain on the plantar fascia.
- Avoid going barefoot on hard surfaces to prevent excessive stress on the feet and minimize the risk of injury.
- Regularly trim toenails, keep feet clean and dry, and moisturize to prevent skin issues and maintain overall foot health.
Connection Between Plantar Fasciitis and Heart Disease

Research suggests that there may be a connection between plantar fasciitis and heart disease. While the direct link is not fully understood, studies have shown that individuals with cardiovascular issues may be more prone to developing foot conditions like plantar fasciitis.
Impact of Cardiovascular Health on Foot Conditions
Cardiovascular health plays a crucial role in overall well-being, including the health of our feet. Poor circulation, a common issue in individuals with heart disease, can affect the delivery of nutrients and oxygen to the feet, leading to conditions like plantar fasciitis.
- Individuals with heart disease should pay attention to their foot health and seek treatment for any foot pain or discomfort.
- Managing cardiovascular risk factors, such as high blood pressure and high cholesterol, can also help improve foot health and potentially prevent conditions like plantar fasciitis.
- Regular exercise and maintaining a healthy weight are essential for both heart health and foot health.
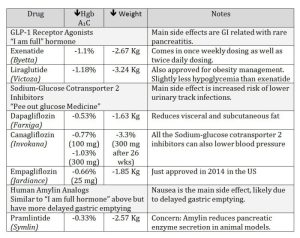
Plantar Fasciitis and Health Diabetes
Plantar fasciitis and diabetes are two health conditions that can have a significant impact on foot health. The relationship between the two conditions is crucial to understand, as diabetes can influence the development and management of plantar fasciitis.
Impact of Diabetes on Foot Health
- Diabetes can lead to nerve damage, known as peripheral neuropathy, which can result in a loss of sensation in the feet. This can make diabetic individuals more susceptible to foot injuries and conditions like plantar fasciitis.
- Poor circulation due to diabetes can also slow down the healing process of foot injuries, including plantar fasciitis. This can prolong the recovery time and increase the risk of complications.
- High blood sugar levels in diabetes can weaken the immune system, making it harder for the body to fight off infections that may arise from untreated plantar fasciitis.
Managing Plantar Fasciitis in Diabetic Individuals
- Diabetic individuals with plantar fasciitis need to work closely with healthcare providers to develop a comprehensive treatment plan that takes into account their diabetes management.
- Monitoring blood sugar levels regularly and maintaining a healthy lifestyle with proper nutrition and exercise can help improve overall foot health and support the healing process of plantar fasciitis.
- Special considerations may need to be made for diabetic individuals when it comes to medications and therapies for plantar fasciitis, to ensure they do not interfere with diabetes management.
Preventive Strategies for Diabetic Patients
- Diabetic patients can reduce the risk of developing plantar fasciitis by wearing supportive footwear, maintaining a healthy weight, and engaging in regular foot care practices.
- Avoiding prolonged periods of standing or walking, especially without proper support, can help prevent excess strain on the feet and reduce the likelihood of developing plantar fasciitis.
- Regular foot exams by healthcare providers can help diabetic individuals identify any potential issues early on and take preventive measures to protect their foot health.
Plantar Fasciitis and Eating Disorders
Eating disorders can have a significant impact on the development and management of plantar fasciitis. The nutritional deficiencies associated with eating disorders can affect foot health and worsen symptoms of plantar fasciitis. It is essential for individuals with eating disorders to address foot-related issues like plantar fasciitis while managing their overall health.
Nutritional Deficiencies and Foot Health
Nutritional deficiencies commonly associated with eating disorders, such as inadequate intake of essential vitamins and minerals, can lead to weakened bones and muscles in the feet. This can increase the risk of developing conditions like plantar fasciitis, as the plantar fascia becomes more susceptible to inflammation and injury.
- Nutritional deficiencies like low levels of Vitamin D and calcium can weaken bones and contribute to foot pain and inflammation.
- Inadequate protein intake can impair muscle strength and recovery, leading to increased stress on the plantar fascia.
- Dehydration, a common issue in eating disorders, can reduce the elasticity of tissues in the feet and exacerbate symptoms of plantar fasciitis.
Recommendations for Managing Plantar Fasciitis with Eating Disorders
It is crucial for individuals with eating disorders to prioritize their overall health while addressing foot-related issues like plantar fasciitis. Here are some recommendations for managing plantar fasciitis in the context of eating disorders:
- Work with a healthcare provider to develop a balanced meal plan that includes essential nutrients for foot health, such as vitamins, minerals, and protein.
- Incorporate gentle stretching and strengthening exercises for the feet to improve flexibility and reduce the risk of plantar fasciitis flare-ups.
- Stay hydrated and ensure adequate fluid intake to support tissue elasticity and reduce inflammation in the feet.
- Seek professional help for the eating disorder to establish healthy eating habits that promote overall well-being, including foot health.
Concluding Remarks

Bid farewell to foot pain as you arm yourself with knowledge on the best treatment options for Plantar fasciitis. Say hello to happy, healthy feet once again!
Popular Questions
Can plantar fasciitis be cured completely?
While it can be managed effectively, complete cure is not always guaranteed. Consistent treatment and care can help alleviate symptoms.
Are orthotic devices necessary for treating plantar fasciitis?
Orthotic devices can provide support and relief, but they may not be essential for every individual. Consult with a healthcare provider for personalized advice.
Is surgery the only option for severe cases of plantar fasciitis?
Surgery is usually considered when non-surgical methods have not provided relief. It’s important to explore all treatment options before opting for surgery.